Antibiotic Resistant Bacteria – A Threat to Food Safety
ABSTRACT:
The use of antibiotics and the frequency of their use to curb infectious diseases have been increasing. This has resulted in the build-up of antibiotic-resistant bacteria causing a big threat to food safety.
The build-up of resistance is a natural process and therefore extensive focused research is required with respect to characteristics of a bacteria and their response to inactivation mechanism. It is also important to gain information on the mechanism action of these microbes to understand how they spread the resistance.
The ever-growing outbreaks related to the foodborne pathogens and food product recalls worldwide, explains the importance of controlling pathogens in food.
To top it all, resistance build-up in a pathogen has created new challenges for the food industry to produce safe food.
This paper explains mechanism of the resistant spread of bacteria, the spread of resistance of bacteria in the food chain, the role of food in spreading the antibiotic resistant food-borne pathogens and the control measures required to prevent the anti-microbial resistance.

INTRODUCTION
The concept of antibiotic resistance bacteria was first explained in the 1940s (Capita and Carlos., 2012). Thereafter the use of antibiotics to curb infections and diseases has only increased considering its efficiency to solve health crisis.
Antibiotic resistance occurs naturally in a bacterium that results in rendering the technologies ineffective used for killing and inactivation of the bacteria (WHO.,2018). There have been warnings about the misuse or overuse of these antibiotics which may lead to resistance build-up in the bacterium strains on which it is used.
After just a year of widespread use of Penicillin, some strains of Staphylococcus aureus became resistant to Penicillin (Alanis.,2005). If certain bacterial strains develop resistance, it becomes extremely complex to eliminate them from the body and thus can prove to be fatal.
The antimicrobial strains develop a progeny through adaptation that is generally caused by mutation or through ingesting genetic material through other bacterial strains (FVE.,2002).
There is horizontal and vertical sharing of genetic material among the bacteria and this accelerates the antimicrobial resistance build-up from non-pathogenic microbes to pathogenic microbes.
For instance, In case of biofilms where a cluster of bacteria forms a film on a food product, it becomes difficult to disrupt this layer given the adaptive stress response of the bacteria and poor penetration power of the available antibiotics.
The chemical disinfectants are also unsuccessful in breaking this biofilm. Such situations demand the emergence of new therapeutic agents (Stewart.,2001)
MECHANISM OF THE ANTIMICROBIAL STRAINS:
The resistance of bacteria towards a certain antibiotic is based on the internal factors of its physiology and different characteristics. The bacteria can also use their survival strategy to express and suppress their genes which are called as the stress response systems.
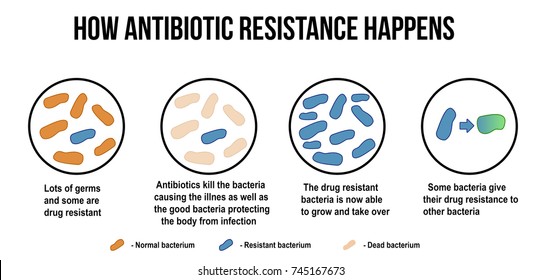
Generally, when the use of antibiotic consumption increases where it is not required and intake is done also in cases where the infection has not been caused by bacteria, there are chances of resistance build-up for the antibiotic as the bacteria gets adapted to its frequent use.
The spread of the resistant bacteria in the human body is caused as bacteria in the body are killed by the antibiotics but the resistant strains remain and multiply in the body by sharing their resistance.
The presence of integrons in bacteria facilitates the share of resistance to other bacteria as integrons help the bacteria to evolve (David et al.,2001).
BACTERIAL RESISTANCE SPREAD IN THE FOOD CHAIN
There has been evidence of transfer of the bacteria in the food chain from plants to animals and from animals to humans. The transfer is also possible from plants to humans, by way of the bacteria sharing the resistant genetic material amongst themselves.
In order to protect the livestock from various infections, different antibiotics are used. Antibiotics like nourseothricin and oxytetracycline are used in the animal feeds and thus the resistance can spread from the faecal flora to the gut flora of the humans working with the livestock (Molbak.,2004).
These gut florae that acquire the resistance in humans can further cause infections in the urinary tract as the virulent bacterial species have a higher chance of acquiring the resistance. (SundsfJord et al.,2001).
Fresh fruits and vegetables in a farm can also be contaminated by resistant bacterial strains through the soil they grow in, that has already been contaminated with animal or human faeces.
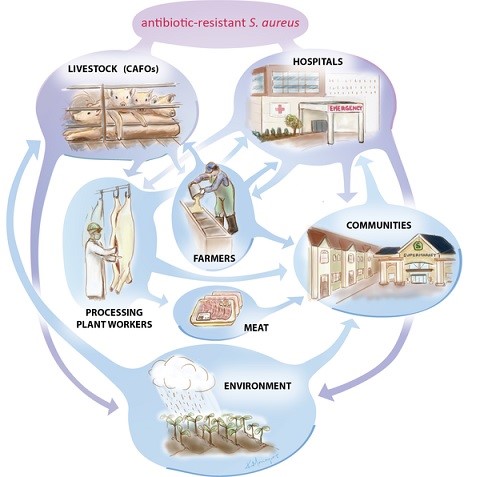
The resistance bacteria can also spread among humans through touch, coughing, sneezing etc.,
Fig 1 below depicts the spread of bacterial resistance through various sources (Desai R, 2016).
The following Table describes the source of some known antibiotic resistant bacteria, the illnesses caused by them and the antibiotics they are resistant to:
| Antibiotic Resistant Bacteria | Illness | Source | Antibiotic |
| E coli | Urinary Tract Infection, Respiratory Tract Infections, Intestinal Illness, Wound infections | Contaminated food and water, Direct contact with a sick person | All types of Antibiotics mainly fluoroquinolone (WHO.,2018) |
| Campylobacter Jejuni | Intestinal infections | Contaminated food or water and animals | Quinupristin, Dalfopristin (McDermott et al.,2006) |
| Enterobacteriaceae | Intestinal infections | Contaminated food and water | Carbapenem (Gov of Canada) |
| Staphylococcus aureus | Various infections of bloodstream, bones and lungs | Contaminated food and water mainly the meat industries | Methicillin (Gov of Canada) |
| Salmonella | Diarrhoea, Vomiting, Stomach Cramps, Fever | Contaminated food and water, Direct contact with infected animals | Commonly used antibiotics mainly ceftriaxone in children and cetrioxone in adults, streptomycin, trimethoprim, amikasin, apramycin, nalidixic (David et al.,2001) |
| Enterococci | Intestinal illness | Healthcare facilities | Vancomycin (Gov of Canada) |
| Clostridium difficile | Infectious Diarrhoea | Healthcare facilities | Multidrug resistant |
| S.Enterica Serotype typharium | Severe infections | Meat and meat products producing industries. | Multidrug resistant |
| Coliform | Severe infections | Contaminated food and water and person to person | Multidrug resistant |
ROLE OF FOOD IN SPREADING THE ANTIMICROBIAL RESISTANCE
As it can be observed from Table no 1, it is evident that most of the bacteria known to be antibiotic-resistant are majorly occurring in contaminated food and water and through animals and therefore it can be concluded that resistance is mostly seen in the foodborne pathogens and thus is a challenging situation for the food industries.
Preservation of food from pathogens through inactivation and killing is a major step in food production in order to produce safe and better-quality food products for the consumers. There have been outbreaks in the past across the globe, due to various pathogenic bacteria because of gaps in the inactivation system, in the food processes.
Resistance build-up in the bacteria has elevated this challenge making it more difficult to inactivate them. This has brought about the emergence of new technologies in the food sector for their isolation and prevention in food. Industries are making an effort to use advance methods of isolating the resistant strains of the bacterium and then working towards their inactivation.

Deriving results from a research based on isolation of resistant Salmonella strains from ground meat, it was observed that 83 % of the isolated strains showed resistance to at least one antibiotic and 53% of the strains showed resistance to at least three antibiotics (David et al., 2001).
The isolation of the strains was done by serotyping, phage typing and pulsed-field gel electrophoresis. It was observed that 20% of the ground meat samples collected from the supermarket had resistant bacterial strains in them. This forces us to look upon the re-evaluation of antibiotic use on animals that are bred for diets.
Research has proven that strains of certain bacteria like the Enterococcus faecium can be observed in stools of the individuals ingesting the resistance strains through consumption of contaminated chicken and pork for 14 days after consumption.
The estimation is 40 CFU per g of stool is observed, which is huge. E. faecium is capable of withstanding low pH values in the gut and is glycopeptide resistant (Sorensen.,2001). Presence of these strains in the faecal matter in such high numbers creates a huge risk of their spread if hygiene and sanitation practices in a food facility are compromised.
Prevalence of resistant bacteria has also been observed in the Soils and Vegetables after harvest. Vegetables like tomato, cucumber, pepper, carrot have been evaluated to show strains of resistant bacteria like Coliform and Clostridium perfringence.
When faecal matter from the animals is used as a manure to fertilize the soil the resistance is transferred via the soil to the vegetables and thus through the vegetables to humans (Marti et al.,2013).
The bacterial count in the soil calculated was higher than that of the vegetables. Artificially added microorganisms in food processing like the probiotics and genetically modified foods also can transfer antimicrobial resistance to the consumer (Capita and Carlos.,2012).
Moreover, in food industries to keep the food safety intact antimicrobial agents in various forms like preservatives, disinfectants and decontaminants are used in every stage of food processing.
Given the increased use of antibiotics and their disadvantages due to higher use, it is important to develop strategies and preventive measures to limit their use.
PREVENTIVE MEASURES:
Following strategies have been put into action by the Canadian Government to work towards antimicrobial resistance:
- Monitoring and Surveillance – Keeping a track of the affected population so that a track record of the growing numbers is maintained, and prompt action can be taken when necessary. The Canadian Antimicrobial Surveillance Systems (CARSS) is a system that helps in gathering information about antimicrobial resistance in humans and animals. The World Health Organization is also making a continuous effort to support countries globally to establish efficient surveillance systems (WHO.,2013)
- Establishing Strict Regulations and Guidelines on the use of antibiotics and making the population aware of the use of veterinary drugs in order to keep the consumption in control. The Federal Action Plan for Antimicrobial Resistance and Use in Canada was established in the year 2015 by agencies like Health Canada, CFIA, Agriculture and Agrifoods Canada, National Research Council Canada and Public Health Agency of Canada (Federal Action Plan.,2015)
- Keeping the sales record of antibiotics sold and ensuring its allowance only based on the prescription
- Developing new and innovative antibiotic resistance by supporting research for antimicrobial resistance. The government is trying to create a uniform platform for different sectors like the hospitals, industries and agricultural sectors to come together to collectively work on vaccine development and disease prevention and treatment
- As we are aware that most of the foodborne pathogens like Salmonella and Campylobacter enter the food chain from the beginning of the food chain which is the farm. Therefore, it is important to have food safety programs implemented at the farm where the farmers are trained about sanitation and hygiene practices. They must be educated about the use of only authorized antimicrobials in feed and food production. (Government of Canada.,2015)

CRITICAL DISCUSSION:
As Vegetables are consumed daily by individuals, the prevalence of resistant bacteria in them makes an individual directly exposed to them. As the various research calculations discussed in the paper evaluated that resistant strains have been isolated from the ready to be sold supermarket food samples, it is essential to consider the amount of human exposure to unsafe food.
Thus the practice of protecting the plant from antimicrobial resistance is as important as protecting it from various pathogens and infections during its growth. Use of antibiotics on animals within short intervals to improve its various qualities results in increased resistance in them and thus population with pets are also at risk of acquiring this bacterial resistance.
CONCLUSION:
The studies show that there has been increased dependence on antibiotics for various purposes right from animal husbandry, agriculture, food processing, health facilities and preservation and storage of food commodities.
However effective their use may prove to be it is essential to limit their use and look for alternative techniques to prevent the fate of these antibiotics turning ineffective and thus rendering an individual susceptible to pathogenic bacteria.
REFERENCES
- David G. White, P. D., Shaohua Zhao, D.V.M., Ph.D., Robert Sudler, M.S., Sherry Ayers, Sharon Friedman, B.A., Sheng Chen, D.V.M., Patrick F. McDermott, Ph.D., Shawn McDermott, B.S., David D. Wagner, Ph.D., and Jianghong Meng, D.V.M., Ph.D. (2001). The Isolation of Antibiotic-Resistant Salmonella from Retail Ground Meats. The New England Journal of Medicine. doi:10.1056/NEJMoa010315
- Desai, D. R. (2016). ANTIMICROBIAL RESISTANCE (AMR). Retrieved from http://drrajivdesaimd.com/2016/11/20/antimicrobial-resistance-amr/
- Federal Action Plan on Antimicrobial Resistance and Use in Canada: Building on the Federal Framework for Action, (2015).
- J, A. A. (2005). Resistance to antibiotics. https://www.ncbi.nlm.nih.gov/pubmed/16216651
- P. F. McDermott , S. Z., D. D. Wagner , S Simjee , R. D. Walker & D. G. White. (2006). THE FOOD SAFETY PERSPECTIVE OF ANTIBIOTIC RESISTANCE. Animal Biotechnology. doi: https://doi.org/10.1081/ABIO-120005771
- Romain Marti, A. S., Yuan-Ching Tien, Roger Murray, Lyne Sabourin, Yun Zhang, Edward Topp. (2013). Impact of Manure Fertilization on the Abundance of Antibiotic-Resistant Bacteria and Frequency of Detection of Antibiotic Resistance Genes in Soil and on Vegetables at Harvest. American Society for Microbiology. doi:10.1128/AEM.01682-13
- Rosa Capita, C.-A. C. (2012). Antibiotic-Resistant Bacteria: A Challenge for the Food Industry. Critical reviews in food science and nutrition, 53(1). doi:https://doi.org/10.1080/10408398.2010.519837
- S.Stewart, P. (2002). Mechanisms of antibiotic resistance in bacterial biofilms. International Journal of Medical Microbiology. doi:https://doi.org/10.1078/1438-4221-00196
- Thomas Lund Sørensen, M. D., Marianne Blom, M.Sc., Dominique L. Monnet, Ph.D., Niels Frimodt-Møller, M.D., D.M.Sc., Rikke Lykke Poulsen, Ph.D., and Frank Espersen, M.D., D.M.Sc. (2001). Transient Intestinal Carriage after Ingestion of Antibiotic-Resistant Enterococcus faecium from Chicken and Pork. The New England Journal of Medicine. doi:10.1056/NEJMoa010692
- WHO. (2013). Antimicrobial resistance: conserving life-saving medicines takes everyone’s help. https://www.who.int/features/2013/amr_conserving_medicines/en/
- WHO. (2018). Antimicrobial resistance. https://www.who.int/en/news-room/fact-sheets/detail/antimicrobial-resistance



