
Listen To Your Gut Microbiome!
What is Microbiome?
A microbiome is the community of microorganisms living together in a particular habitat. Human guts, animals, and plants have their unique microbiome, but so do soils, oceans, and even buildings.
Microbiome present in humans is called as “Human microbiome.” The human microbiome is the aggregation of all microbiota that resides on or within any of several human tissues and biofluids, including the skin, mammary glands, placenta, seminal fluid, uterus, ovarian follicles, lung, saliva, oral mucosa, conjunctiva, biliary and gastrointestinal tracts.
Humans are superorganisms or ‘‘holobionts’’ composed of 10% human cells and 90% microbial cells. The body contains at least 1000 different species of known bacteria and carries 150 times more microbial genes than are found in the entire human genome (See fig 1).
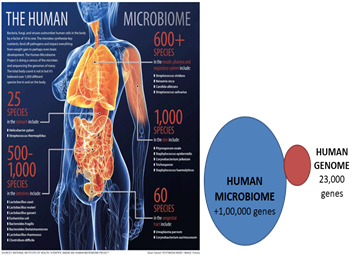
Fig 1. Complexity and importance of human microbiome (Source: national institutes of health, scientific American human microbiome)
The microbial genomes and human genomes (hologenome) have co-evolved. Their metabolism and survival are now wholly intertwined. Human gastrointestinal microbiota (gut flora/gut microbiota) is the microorganisms that live in the digestive tracts of humans.
Humans are the harbors of up to 2 kg of microbes in our gut. Several factors contribute to the shaping of the healthy gut microbiota, and this continues dynamically throughout the life of an individual. They include mode of delivery, age, diet, antibiotics use, etc. This microbiome differs intrapersonally based on age, body site, changes in nutrition and lifestyle of an individual, and hygiene.
What is the role of gut microbiome?
Most of us are conscious that the bacteria in our gut play a vital role in digestion. When the stomach and small intestine are unable to digest certain foods we eat, gut microbes jump in to offer a helping hand, ensuring we get the nutrients we need.
Besides, gut bacteria are known to aid the production of specific vitamins – such as vitamins B and K and play a significant role in immune function. The microbiome is necessary for human development, immunity, nutrition.
The bacteria living in and on us are not enemies but beneficial colonizers. Autoimmune diseases such as diabetes, rheumatoid arthritis, muscular dystrophy, multiple sclerosis, fibromyalgia are linked with dysfunction in the microbiome.
Disease-causing microbes accumulate over time, changing gene activity and metabolic processes and resulting in an abnormal immune response against substances and tissues usually present in the body. Autoimmune diseases appear to be passed in families not by DNA inheritance but by inheriting the family’s microbiome.
But increasingly, researchers are working to find out more about how gut bacteria, particularly the bacteria that is unique to us individually influence our health and risk of disease. Table 1 explains the functions of gut microbiota.
| Functions | Explanation |
| Metabolite production | The fermentation of fibers results in the production of short-chain fatty acids (SCFAs), which are involved in many cellular processes and metabolic pathways, in the enhancement of the gut barrier function and the regulation of the inflammatory responses. |
| Vitamin production | Microbiota produce essential vitamin B12 and vitamin K that humans cannot produce. |
| Influence on epithelial homeostasis | Microbiota promotes gut epithelial integrity by the production of mucin protein. |
| Influence on pathogen colonization | Microbiota competes with pathogens for attachment sites and nutrients by competitive inhibition of pathogens. They produce antimicrobial substances (Ex. Bacteriocins). |
What is the role of gut microbiota in health?
The intestinal microbiome influences the body from birth and throughout life by regulating the digestion of food, the immune system, the central nervous system, and other bodily processes.
In recent decades, a tremendous amount of evidence has strongly suggested a crucial role of the human microbiota in human health and disease via several mechanisms.
Any deviation from healthy gut microflora is named as “gut dysbiosis.” Gut dysbiosis may lead to weight gain, obesity, diabetes, cancer. It also affects the gut, brain, and heart health. Figure 3 explains the list of diseases linked with gut dysbiosis.
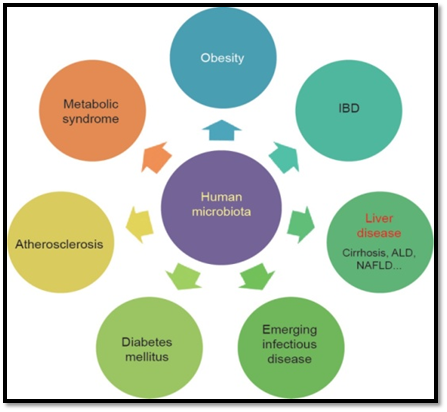
Fig 3. The list of diseases linked with gut dysbiosis (Source: Wang. B et al., 2017)
How is the gut microbiota studied?
Human stool samples will be collected to analyze and characterize the gut microbiota. Culture dependent (serial dilution & plating) and culture-independent (Ex.16S rRNA based metagenomics) methods are used to study the microbiome. Figure 4. Explains culture-independent methods to study the gut microbiome.
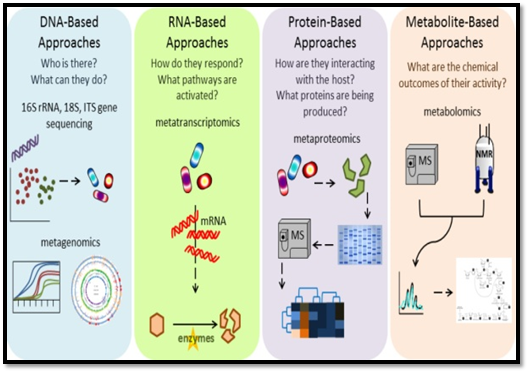
Fig. 4 Culture-independent methods to study the gut microbiome
(Source: Environmental chemicals, the human microbiome, and health risk: A research strategy. National Academies Press)
What are the ways to alter the gut microbiota?
Since the gut microbiome is shaped by the food we eat and the conditions around us, it makes sense that there are methods to make it healthier. A healthy diet can encourage the presence of good gut bacteria.
Exercise may also be vital to improving gut bacteria diversity. Gut microbiota can be shaped through passive strategy or active strategy. The former includes diet, lifestyle, environment, while the latter comprises pre- and probiotics, and Fecal Microbiota Transplantation (FMT). Figure 5. depicts the startup companies worldwide based on the microbiome.
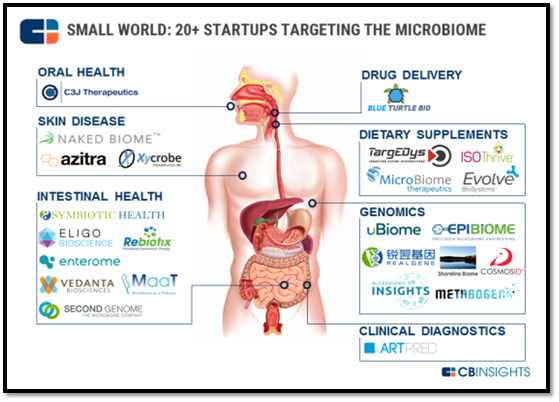
Fig. 5 Startup companies worldwide based on the microbiome
Potential therapies aimed at the modulation of the intestinal microbiota
Probiotics: Live microorganisms that, when given in adequate amounts, provide a health benefit on the host. Examples include strains of the genera Bifidobacterium and Lactobacillus.
Probiotics can have multiple interactions with the host, including competitive inhibition of other microbes, effects on mucosal barrier function, and interaction with antigen-presenting dendritic cells.
Prebiotics: A selectively fermented ingredient that results in specific changes in the composition and/or activity of the gut microbiota, thus conferring benefits upon host health. Prebiotics are usually non-digestible carbohydrates, oligosaccharides, or short polysaccharides, with inulin, oligofructose, galactofructose, galacto-oligosaccharides, and xylo-oligosaccharides being some of the most intensively studied.
Fecal microbiota transplantation: The introduction of gut bacteria from a healthy donor into a patient, through the transfer of an infusion of a fecal sample via nasogastric tube, nasoduodenal tube, rectal enema or the biopsy channel of a colonoscopy. Figure 6 describes the effect of fecal microbiota transplantation from obese and lean twins to germ-free mice.
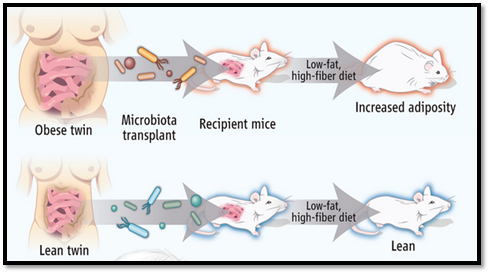
Fig. 6 The effect of fecal microbiota transplantation from obese and lean twins to germ-free mice. (Source: Walker and Parkhill, Science, 2013)
Germ-free mice inoculated with microbiota from obese or lean human twins take on the microbiota characteristics of the donor. Those receiving the obese microbiota (red outline) had an increase in adiposity, whereas those receiving the lean microbiota (blue outline) remained lean.
Here are some issues researchers are studying:
• How is a particular microbiome built in an individual? Does it vary over time?
• How do the human and microbe community communicate?
• How does a specific combination of microbes affect nutrition? How do variations in diet alter the microbiome?
• How does the microbiome affect immunity and lead to disease?
• How do antibiotics alter the microbiome? Conversely, how do the microbes in our bodies influence how we react to various drugs?
• How can a microbiome be modified to enhance health?
Conclusion:
As life expectancy continues to increase, it is essential that we understand how best to maintain good health. Following the complicated link among what we choose to eat, activity levels, and intestinal microbiota richness is essential.
Developing new approaches to manage the beneficial properties of our microbiota by finding ways to integrate health-promoting features into modern living should be the goal. The human microbiome is the biggest thing in biology after the human genome project with extraordinary human health implications.
It can provide simple, sustainable, and safer solutions for human health not possible earlier, and it is a potent tool for personalized therapies when used in conjunction with the human genome. There are many definitions for the gut microbiome.
But, I would like to refer our gut microbiome as an internal micro pet which is unique to all of us. If we rear and take care of them properly in turn, they will give us numerous benefits. Listen to your internal micro pet! Stay healthy!
References:
- Mindell, D.P. (1992). Phylogenetic consequences of symbioses: Eukarya and Eubacteria are not monophyletic taxa. Biosystems, 27 (1), 53–62. PMID:1391691
- Lederberg, J. (2000). Infectious history. Science, 288 (5464), 287–293. PMID:10777411
- National Academies of Sciences, Engineering, and Medicine. (2018). Environmental chemicals, the human microbiome, and health risk: A research strategy. National Academies Press.
- A. W. Walker., J., Parkhill. (2013). Microbiology-Fighting obesity with bacteria.Science, 341(6150), 1069-70. doi: 10.1126/science.1243787.
- Wang, B., Yao, M., Lv, L., Ling, Z., & Li, L. (2017). The human microbiota in health and disease. Engineering, 3(1), 71-82.
- https://depts.washington.edu/ceeh/downloads/FF_Microbiome.pdf Accessed on: 29.7.19
Suggeted reading
https://foodtechpathshala.com/antibiotic-resistant-bacteria-a-threat-to-food-safety/
Featured photo credit: Kateryna Kon/Shutterstock.com & Bodenstein Lab



